How To Get Enough Vitamin D
As of 2014, experts predicted that about 1 billion people worldwide have low levels of vitamin D or a deficiency making it one of the most common vitamin deficiencies. If you suspect you are low in vitamin D, you should ask your doctor for a test. This way you can make sure you are supplementing the right levels if you do need more. Always ask your doctor before starting a new supplement.
The recommendation for vitamin D for adults is between 600-800 IU, although that number is up for debate among the science and medical community.
There are three ways to get vitamin D: through food , from direct sun exposure on your skin and through supplements.
Vitamin D Improves Immune Function In Immunosuppressant Mice Induced By Glucocorticoid
This article is mentioned in:
Abstract
Introduction
Vitamin D is an essential fat-soluble vitamin withmultiple functions. The main source of vitamin D is transformedfrom 7-dehydrocholesterol after exploration with ultravioletirradiation and sequential hydroxylation into 25D and an activehormone, 1,25-dihydroxy-vitamin D3, by hydroxylases in the kidneyand liver. It can also be absorbed from dietary intake or oralsupplements. It has been shown that vitamin D receptor ishighly expressed in the intestine, kidney, thyroid and bone. Previous findings showed thatseveral types of immune cells such as T lymphocytes, monocytes,macrophages, and dendritic cells express VDR as well. The activeform of vitamin D exerts its effects on these tissues by binding toVDR. In addition, some studies present that macrophages, dendriticcells and lymphocytes also express vitamin D activating enzyme,1–hydroxylase . Therefore, except for the classicalphysiological function of regulation of calcium and bonemetabolism, vitamin D may also have immunomodulatory effects.
Materials and methods
Reagents
Animal studies
Proliferation assay ofsplenocytes
Quantification for IL-2production
Flow cytometric analysis of cellmarkers of CD4 and CD8
Results
Vitamin D And Autoimmune Conditions
Deficiency in vitamin D is also associated with higher rates of autoimmunity, and this may be due to its effect upon immuno-modulatory T-cells.
Autoimmune diseases including multiple sclerosis, rheumatoid arthritis, alopecia areata , and lupus are impacted by the function of T-cells and vitamin D deficiency.
Now, this doesnt mean that vitamin D will protect you from developing autoimmunity, or from experiencing a flare-up, but we do know that adequate vitamin D levels benefit the healthy function of immune cells, which in turn decreases risk for autoimmunity.
This is why your functional medicine provider at CentreSpringMD will test for nutrient deficiencies when working with you to get your autoimmunity into remission.
Also Check: What Is The Best Vitamin For Men Over 50
Vitamin D Adaptive Immunity And Human Disease
Although the adaptive immune system is essential for much of the innate immune activity outlined in previous sections, it clear that vitamin D may also be linked to diseases more closely associated with T- and B-cell function. In particular, increasing numbers of studies have linked vitamin D insufficiency to increased risk or severity of autoimmune disease. Low vitamin D status has been linked to type 1 diabetes, and supplementation with vitamin D has been reported to protect against this disease. In a similar fashion, analysis of the NOD mouse, an animal model for type 1 diabetes, has shown increased disease severity under conditions of dietary vitamin D restriction. Another strand of evidence linking vitamin D with type 1 diabetes is provided by the extensive genetic analyses that have investigated the physiological impact of polymorphic variations in the genes for various components of the vitamin D metabolic and signalling system. Specific VDR gene haplotypes appear to protect against diabetes, and polymorphisms in the CYP27B1 gene have also been shown to affect diabetes susceptibility.
Safety Of Supplementation In Humans

Recommendations from national health authorities for optimal serum 25D levels differ in many countries . Currently, no international consensus is available on the optimal level for vitamin D supplementation, in particular on the safe upper level. While the tolerable upper daily limit given by the Endocrine Society is 10,000 IU , the more conservative Institute of Medicine considers a supplementation of up to 4000 IU/day to be safe . The European Food and Safety Authority currently recommends to stay below 4000 IU/day .
Administration of the highly active metabolite calcitriol is limited because of potential side effects, in particular hypercalcemia. Active vitamin D or its analogs are rarely required except in advanced chronic kidney disease and very few other indications such as hypoparathyroidism and pseudohypoparathyroidism. The most common forms of inactive vitamin D used for supplementation are cholecalciferol and ergocalciferol , shown in Table 1. While in a recent meta-analysis vitamin D3 has been found to be more efficacious in improving 25D status, especially when given as loading doses , both forms are considered to have an excellent safety profile including a broad therapeutic window .
Recommended Reading: Does Vitamin D3 Help You Lose Weight
Risks Of Getting Too Much Vitamin D
If you take excessive amounts of vitamin D supplements, you may get too much of it. However, this is unlikely to happen through diet or sun exposure because your body regulates the amount of vitamin D produced through sun exposure.
Vitamin D toxicity can lead to an increase in your blood calcium levels. This can result in a variety of health issues, such as (
Vitamin D And Type 1 Diabetes Mellitus
Type 1 Diabetes Mellitus is an autoimmune disease with T cell mediated destruction of pancreatic -cells. It is hypothesized that Vitamin D supplementation early in life could be protective therapy against the development of T1DM . Vitamin D supplementation in the first year of life in children produced a 33% risk reduction of developing T1D in a subgroup analysis of the EURODIAB study . A meta-analysis of four clinical studies also revealed a significantly reduced risk of development of T1D among infants receiving vitamin D supplementation . Many trials on vitamin D and T1D are currently ongoing which will hopefully expand our understanding of this topic.
Don’t Miss: Where To Get Vitamin D
Vitamin D Analogue Treatment
Vitamin D analogues have also shown outstanding efficacy in IBD treatment. The analogue, KH 1060, inhibits PBMC proliferation, downregulates TNF-, and synergizes with anti-TNF- biologicals to treat IBD.162 Intracellular adhesion molecules and matrix metalloproteinases are up-regulated in the mucosa of IBD patients and play an important role in recruiting leukocytes to sites of inflammation. In addition, inflammatory cytokines such as TNF- and IL-1 can induce ICAM-1. The vitamin D analogue, ZK 156979, reduces MMP production and ICAM-1 and LFA-1 levels in PBMCs from IBD patients and could serve as a potential IBD treatment strategy.163 The vitamin D form, 1.252D3, and its analogue, EB 1089, inhibit PBMC proliferation, induce apoptosis of PBMC from healthy individuals and IBD patients, and downregulate ICAM-1 expression.164 These results demonstrated that vitamin D analogues play a critical role in suppressing mucosal inflammation during IBD likely by inhibiting the recruitment of leukocytes and production of pro-inflammatory cytokines at sites of inflammation.
Vitamin D And Innate Immunity
Vitamin D differentially modulates monocyte, macrophage, and dendritic cell molecular responses to innate immune stimulation.34 Almost a quarter of primary vitamin D targeted genes in monocytes are related to immune modulation.35 In vitamin D deficient individuals D3< 26ng/mL in this study), VDR expression in monocytes was decreased in a concentration-dependent manner in spite of an increase in monocyte adhesion to the endothelium.36 Monocyte-platelet aggregates , markers for platelet activation, were elevated in vitamin D deficient individuals suggesting a pro-inflammatory monocyte phenotype in vitamin deficiency.36 In addition, normal vitamin D levels are enough to inhibit LPS-induced p38 activation and interleukin-6 and tumor necrosis factor- production in human monocytes.37 Besides, vitamin D could downregulate the expression of Toll-like receptor 9 and inhibit its subsequently secreted IL-6 after stimulated with a TLR-9 agonist in monocytes.38
Vitamin D not only inhibits DC differentiation and maturation43 but also represses inflammation-related signaling pathways in DCs. This includes the inhibition of innate NF-B and p38 mitogen activated protein kinase signaling in monocyte derived DC that have been stimulated with LPS.34
Read Also: Neutrogena Rapid Tone Repair 20 Vitamin C Serum
Vitamin D Helps The Immune System During Cold And Flu Season
Vitamin D helps the immune system stay balanced, much like a gymnist walking a balance beam.
Vitamin D helps our immune systems stay balanced during the cold and flu season, and serve as a pharmacy resource.
There are Vitamin D receptors and activating enzymes on the surfaces of all White Blood Cells. The role that vitamin D plays in keeping the immune system healthy is very complex because the immune system has to be perfectly balanced. If there is too much stimulation, autoimmune diseases can set in. If there is not enough immune system activity, frequent infections can occur.
Low levels of vitamin D have been linked with both extremes, and low levels of vitamin D have been associated with worsening autoimmune diseases. Low levels of vitamin D are not the underlying cause of the autoimmune disease, but low levels of vitamin D can make autoimmune disease states worse.1
Low levels of vitamin D have also been associated with frequent infections. In 2009, the National Institute of Health warned that low vitamin D levels are associated with frequent colds and influenza.2
And so it appears that vitamin D helps keep the immune system balanced much like a gymnast walking on a balance beam.
Since the NIH announcement, there have been many studies to determine the best regimen of vitamin D supplementation and to better understand this association.
References
Related Content:
How Vitamin D Boosts The Immune System
Vitamin D is involved in immunity through several mechanisms and plays a role in regulating both the innate and adaptive immune response in the body. Vitamin D impacts immune health by interacting with vitamin D receptors on innate immune cells throughout the body. The innate immune is the bodys non- specific, first line of defense against foreign pathogens.
Don’t Miss: What Do Prenatal Vitamins Help With
Vitamin D Status And Immune Function
It is important to recognize that most of the genome-wide analyses that have explored the immunomodulatory effects of vitamin D in vitro have focused on treatments using active 1,25D or one of its synthetic analogs. However, as outlined above, pathogen-induction of an intracrine system in cells such as monocytes/macrophages strongly suggests that regulation of immunity in vivo is independent of endocrine, systemic 1,25D. Instead it is likely to be primarily driven by local activation of 25D, the major circulating form of vitamin D and determinant of vitamin D status in any given individual. Thus, it is not surprising that translational studies have focused on the relationship between serum 25D and human immune function, including effects on both innate and adaptive immunity.
Figure 2. Altered gene expression in leukocytes from vitamin D-deficient donors. Peripheral blood mononuclear cells were obtained from 6 healthy donors who had serum 25D levels that were either low or high . After isolation of RNA and generation of cDNA, gene expression analyses in the PBMC samples was carried out by DNA array analyses . Data are shown as genes that were either increased or decreased in low 25D donors relative to high 25D donors .
Vitamin D And Immune Function: An Overview
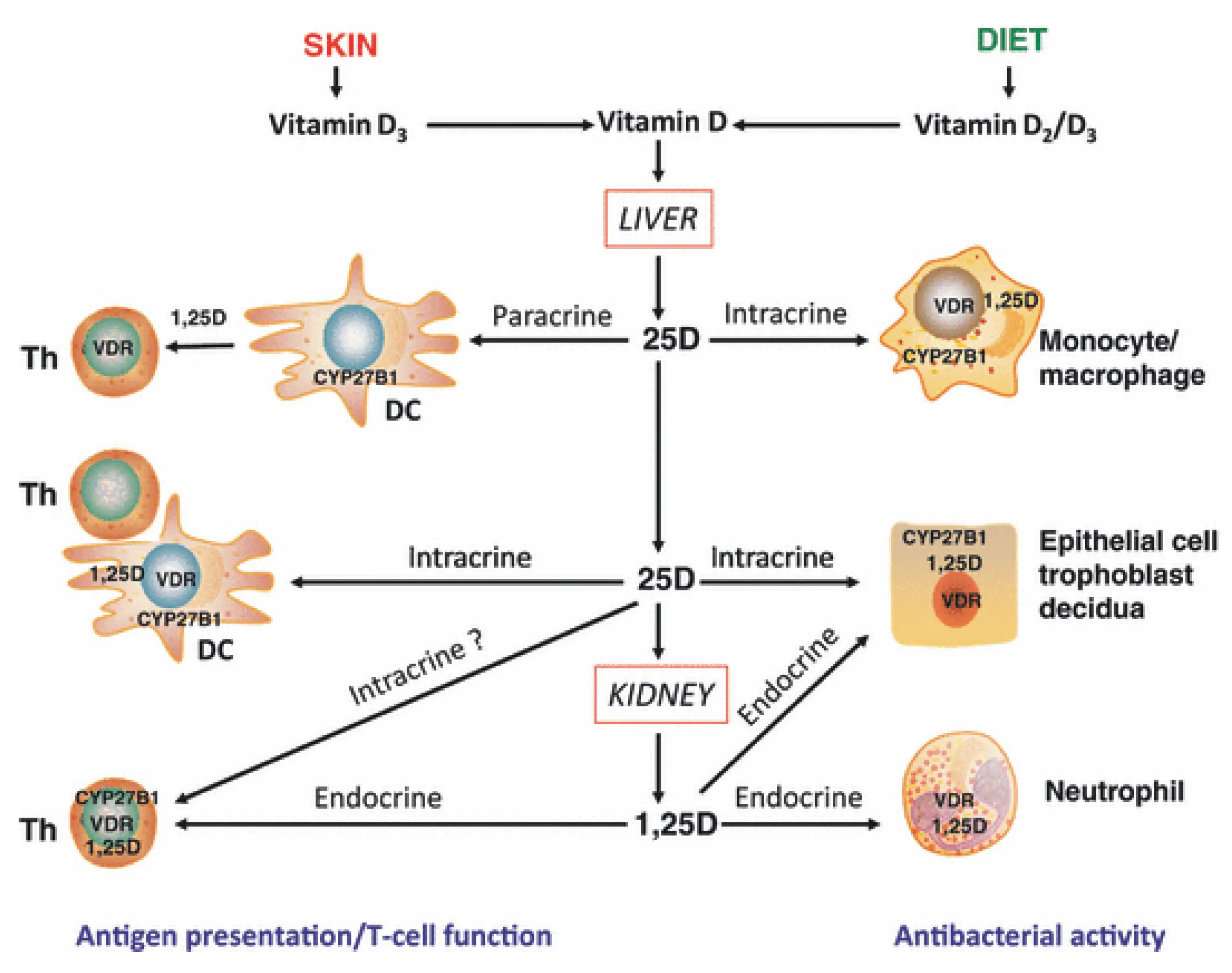
Published online by Cambridge University Press: 18 August 2011
- Affiliation:UCLA and Orthopaedic Hospital Department of Orthopaedic Surgery and the Orthopaedic Hospital Research Center, David Geffen School of Medicine at UCLA, 615 Charles E. Young, Los Angeles, CA 90095, USA
- *
- Corresponding author: Professor Martin Hewison, fax +1 310 825 5409
You May Like: How Much Vitamin D Should I Take In A Day
Impact Of Vitamin D On Immune Function: Lessons Learned From Genome
- 1Department of Orthopaedic Surgery, Orthopedic Hospital Research Center, David Geffen School of Medicine, University of California at Los Angeles, Los Angeles, CA, USA
- 2Division of Dermatology, Department of Medicine, David Geffen School of Medicine, University of California at Los Angeles, Los Angeles, CA, USA
Learn The Role Vitamin D Plays In Immune Health
The ongoing Covid-19 crisis has made us all wonder about the strength of our immune systems, even if we’re vaccinated. As we head into winter, let’s give Vitamin D a moment in the sun and figure out how to use this immune-supporting vitamin to its fullest advantage.
According to recent findings, people with adequate levels of Vitamin D appear to be much less likely to experience severe Covid-19 symptoms. Lets dig into these studies and see what they say, and what it could mean for our own efforts to maintain healthy vitamin D levels for immune support.
Read Also: What Are Prenatal Vitamins Good For When Pregnant
Pandemic Of Vitamin D Insufficiency
Insufficient vitamin D status in humans is becoming more common worldwide.66 Studies on African, European, American, and Brazilian populations support a high prevalence of vitamin D deficiency, and this is more common in urban than rural areas, and in newborns than their mothers.67 Studies indicate that vitamin D prevalence is latitude-related given that serum vitamin D levels are higher in the northern regions of Brazil and the southern regions of China.70,71 In addition, serum 25D levels are not significantly related to gender and age worldwide.72,73
Vitamin D insufficiency is very common among IBD patients, with studies indicating that at least half of patients are vitamin D deficient.20,74 IBD patients have a 64% higher odds of having vitamin D deficiency than healthy individuals,75 and 68% of patients are deficient at diagnosis.76 Low vitamin D status is particularly common among IBD patients with active disease.77
Effects Of Vitamin D Supplementation On Immune Function In Infants
| The safety and scientific validity of this study is the responsibility of the study sponsor and investigators. Listing a study does not mean it has been evaluated by the U.S. Federal Government. Read our disclaimer for details. |
| First Posted : July 8, 2020Last Update Posted : July 8, 2020 |
| Not Applicable |
Study plan to enroll breastfeeding infant at age of 4 month, and provide vitamin D supplement 10 g daily until 6 month. we also enroll 6 month-old infant as control group.
All infants collected 5 ml artery blood and measured vitD nutritional status and immune function. Blood analysis contain complete blood count , differential count , serum calcium, serum Parathyroid hormone , serum 25D3, serum total immunoglobulinE and cell phagocytosis.
Layout table for study information| Study Type : |
| 4 months old or 6 months old breastfeeding infants |
| Masking: |
| Effects of Vitamin D Supplementation on Immune Function in Infants |
| Actual Study Start Date : |
Read Also: What Vitamin Helps Tighten Skin
Signs Of Deficiency And Toxicity
Deficiency
Vitamin D deficiency may occur from a lack in the diet, poor absorption, or having a metabolic need for higher amounts. If one is not eating enough vitamin D and does not receive enough ultraviolet sun exposure over an extended period , a deficiency may arise. People who cannot tolerate or do not eat milk, eggs, and fish, such as those with a lactose intolerance or who follow a vegan diet, are at higher risk for a deficiency. Other people at high risk of vitamin D deficiency include:
- People with inflammatory bowel disease or other conditions that disrupt the normal digestion of fat. Vitamin D is a fat-soluble vitamin that depends on the guts ability to absorb dietary fat.
- People who are obese tend to have lower blood vitamin D levels. Vitamin D accumulates in excess fat tissues but is not easily available for use by the body when needed. Higher doses of vitamin D supplementation may be needed to achieve a desirable blood level. Conversely, blood levels of vitamin D rise when obese people lose weight.
- People who have undergone gastric bypass surgery, which typically removes the upper part of the small intestine where vitamin D is absorbed.
Conditions resulting from prolonged vitamin D deficiency:
Toxicity
Symptoms of toxicity:
- Weight loss
- Irregular heart beat
- Hardening of blood vessels and tissues due to increased blood levels of calcium, potentially leading to damage of the heart and kidneys
Vitamin D And Multiple Sclerosis
MS is an autoimmune disease where T-cells target the central nervous system. The development of experimental autoimmune encephalomyelitis results because of a Th17- and Th1-mediated immune attack on the central nervous system. Other T-cell responses inhibit the development of Th17 and Th1 cells and are therefore important negative regulators of EAE. Negative regulators of EAE include iNKT cells and Treg cells. Patients with MS have fewer iNKT cells and Treg cells and remission from symptoms is associated with the increased number and function of these cell types.
Epidemiological data suggest that there may be a link between vitamin D status and MS in human subjects. Low level of circulating vitamin D was linked to increased disability scores in MS patients. Both sun exposure and vitamin D supplements during childhood and adolescence were shown to correlate with MS incidence north of the Arctic Circle, and these factors were also linked to time of MS onset. Participants in the nurseâs health study who were in the highest quintile of vitamin D intakes had 40% less MS. There is evidence for a role of vitamin D in the aetiology and severity of MS in human subjects.
Don’t Miss: What Does Vitamin D Do For Your Body